Home / Nose Sinuses / Endoscopic Sinus Surgery
Endoscopic Sinus Surgery
Call +65 8125 3580
for 24 by 7 appointment
What is Endoscopic Sinus Surgery?
Functional Endoscopic Sinus Surgery (FESS):
Functional Endoscopic Sinus Surgery is a minimally invasive technique of performing surgery on the sinuses from within the nasal cavity without having to make any external incisions on the face. The technique was introduced in the mid 1980’s. Before that era, surgery on the sinuses was generally performed by making incisions on the face or under the lip. Functional Endoscopic Sinus Surgery has now become the “gold standard” for treating sinus pathology worldwide. Since the introduction of this technique there have been several advances in instrumentations to make this surgery much safer and provide an improved outcome. The surgery may be performed both under local or general anaesthesia depending on the extent and nature of pathology and the choice of surgeon and patient. As the name applies endoscopes are introduced in the nasal cavity to identify the outflow tracts and the opening of the sinuses within the nasal cavity. Using special instruments and techniques, the sinus openings are widened to enable the surgeon to visualise and remove the disease within the affected sinus. The surgery aims to preserve the mucosal lining of the outflow tracts and the function of the sinuses, hence the term “Functional”. Surgery is directed primarily at removing the underlying cause of the disease and is individually tailored. It is based on intricate understanding of the sinus anatomy, as well as normal and altered physiology. The extent of surgery may vary from a minor procedure directed at limited disease, to a radical procedure to involve all the para-nasal sinuses for severe diffuse disease. Over the years, the indications for endoscopic sinus surgery have been expanded to beyond its role as “functional” surgery.
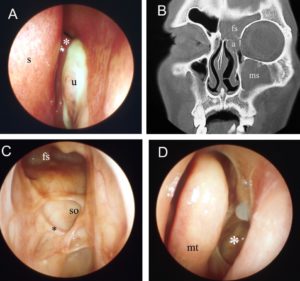
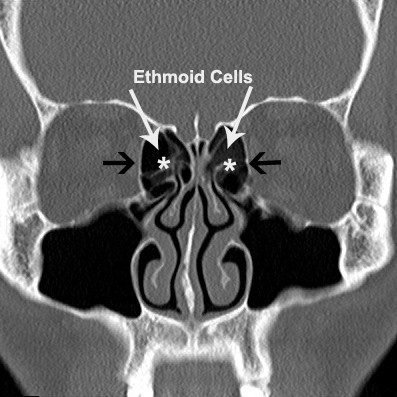
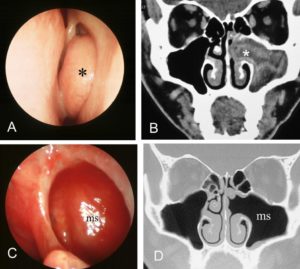
In both cases shown above endoscopic techniques were used. In figure the patient has left maxillary sinusitis documented both on the endoscopic and CT scan of the sinuses shown by the asterisk (Figure 1A and 1B) The endoscope was used to identify the opening of the left maxillary sinus and was widened to drain the pus within the sinus. Postoperative endoscopic examination and CT scan show the widened opening.(Fugure 1C and 1D). In figure 2, the patient’s frontal sinus was also opened from within the nose to drain the pus.
Indications for Endoscopic Sinus Surgery:
- Chronic sinusitis
- Nasal Polyps
- Fungal sinusitis
- Mucoceles of the paranasal sinuses
- Complications resulting from Acute sinusitis such as orbital abscess
- Benign tumours of the nose and sinuses
Extended indications are....Read More
Not sure if endoscopic sinus surgery is you? Speak to A/Prof Sethi to find out if this is the right treatment for you at +65 8125 3580. Or book an appointment with A/Prof Sethi for a consultation on your symptoms and treatment options.
What is the post-operative care after endoscopic sinus surgery?
Postoperative care is essential to maximize the success of the surgery. It is as important, if not more, than the surgery itself. The aim of good postoperative care is to prevent infection, promote mucosal healing and prevent adhesion formation. Adhesions and excessive scarring may narrow or obstruct sinus drainage pathways which were widened during the surgery. This is one of the commonest causes of recurrence of sinus infections after the surgery. Another objective is to look out for any developing complication and deal with it in a timely manner.
My post-operative care protocol after endoscopic sinus surgery is described below:
On the day of the surgery:
Immediately after the surgery while you are still in the recovery room, I will review you to check on your vital signs. Your eyes will be examined for any swelling around the eye. Eye movements, the pupils and vision will be tested. You will also be examined to ensure that there is no excessive bleeding. While in recovery, as you are still recovering from general anesthesia you may not recall this visit.
After about 2-3 hours, I will visit you in the ward by when you will be fully roused. During this visit, I will explain the details of the surgery and intra-operative findings etc. Once again, I will examine you as mentioned above. You may expect some oozing of blood from the nose and the bolster on your nose may require to be changed on a few occasions. Post-operative pain is common. You will be prescribed analgesics to counter the pain. You may experience some discomfort and dryness in the throat as a result of intubation. There is no need to worry about this.
If you have been admitted as a Day Surgery Case, you will be discharged in the evening.
On the 1st Post-operative Day:
Once again a quick examination will be done as mentioned above. Any nasal packing will be removed. Most patients experience a lot of anxiety before the removal of the nasal packing. An anxiolytic and analgesic may be prescribed about an hour before pack removal. There will be some bleeding from the nose following the removal of the packs. This is stale blood that has accumulated in the nose and stops after a few minutes. You may be discharged about an hour after the packs have been removed. After the discharge, I will see you in the clinic to gently vacuum out the blood clots in your nasal cavity.
Subsequent follow up:
Postoperative advice includes, light activity and refrain from blowing the nose too vigorously. Antibiotics, antihistamines, oral steroids and nasal decongestants may be prescribed.
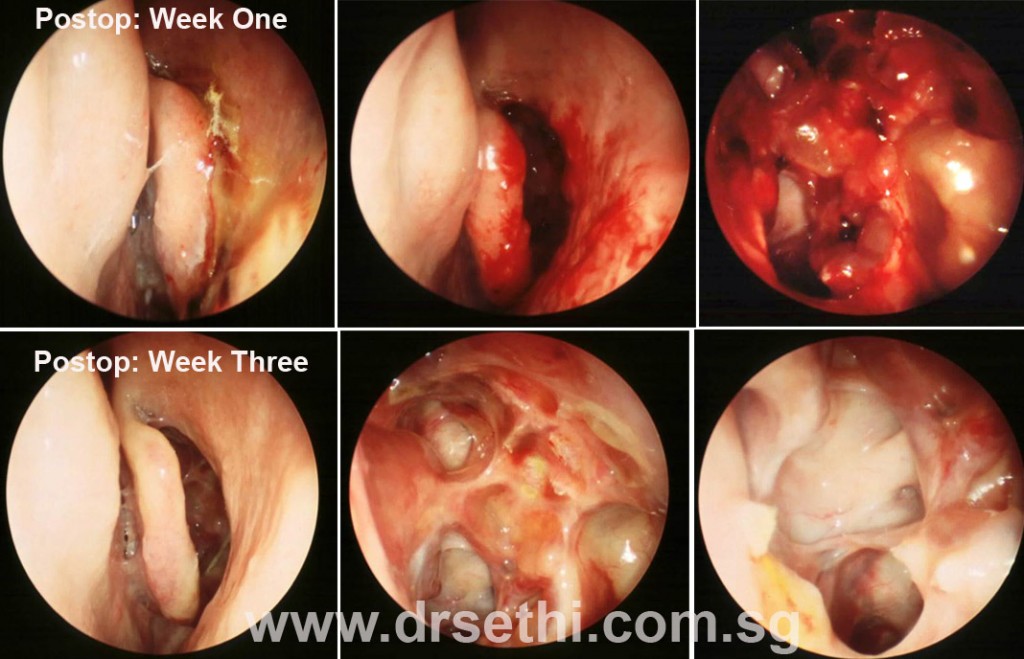
Following that I will see you twice a week for 3 weeks and then once a week for the next 3 weeks.
During each visit the nasal cavity and the sinuses are cleaned with suction to remove stale blood clots, and any crusts formation. Sometimes nasal irrigations may be carried in the clinic. Healing is carefully monitored. If any infection is noted, a culture may be taken so that culture directed antibiotics may be prescribed. If oedema is persistent and severe, a pulse dose of steroids may be prescribed. Frequent nasal irrigations may be necessary.
It takes up to 6 – 8 weeks for the sinus cavities to heal though in some cases it may take even longer. Subsequent appointments are scheduled depending on the progress.
Complications of Endoscopic Sinus Surgery: Orbital (Eye) Complications
Major complications during endoscopic sinus surgery include injury to the orbit, skull base and blood vessels. There complications are, however, rare. Patients have to be informed of these complications so that they are aware of the risks involved and are able to make an informed decision before signing the consent for the surgery. Orbital Complications:
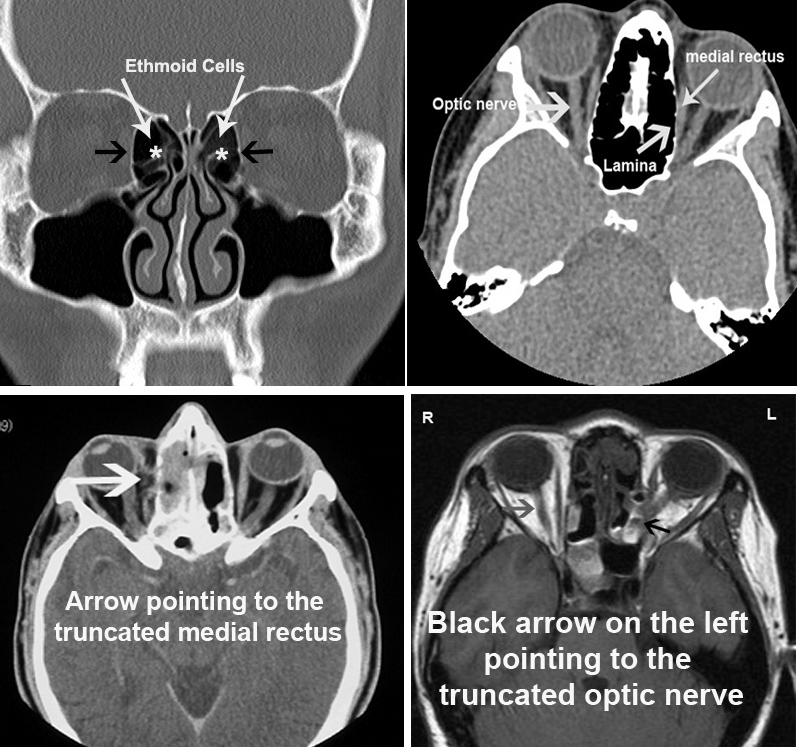
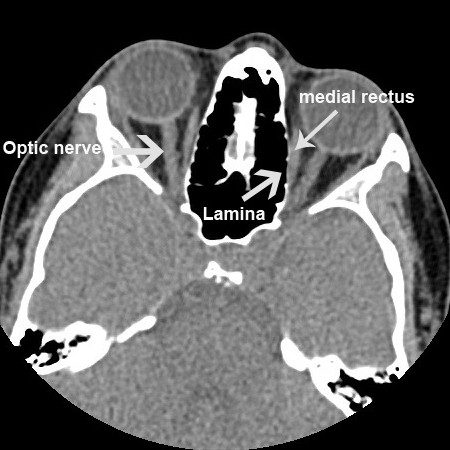
The sinuses are closely related to the orbit (eye socket), which contains the eye globe. The bony partition between the eye and the sinuses is extremely thin. It is called lamina papyrecea, lamina meaning wall and papyrecea means like paper. So, it is literally paper thin. Extreme caution has to be exercised during the surgery to identify this wall and ensure that it is not breached. Unfortunately, in the presence of disease, it may be difficult to identify. The inexperienced and novice surgeons may be a factor. Depending on the extent of the breach, the following orbital complications may result:
- Peri-orbital oedema: mild swelling around the eye particularly over the eyelids may result from a minor breach of the lamina. The vision and eye movements remain normal. The swelling subsides over a few days.
- Orbital hematoma: This is a serious complication where not only the lamina has been breached but there has been internal injury to the orbital fat and blood vessels with in. As a result of bleeding within the orbit, the pressure within the orbit rises, the eye globe protrudes outwards (proptosis) and with increasing pressure the blood supply to the optic nerve may be compromised resulting in blindness.
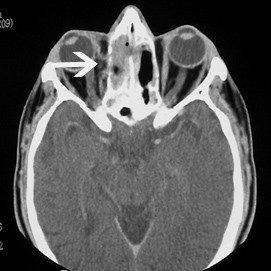
- Extra-ocular muscle injury: The movement of the eye globe are controlled by six muscles called the extra-ocular muscles. One of the muscles, the medial rectus, is very close to the lamina. Injury to this muscle, when the orbit is breached, may result in a partial or complete tear. This may lead to temporary or permanent double vision (diplopia).
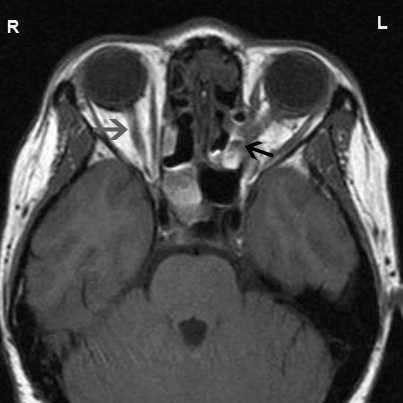
- Optic Nerve Injury: This may result indirectly from orbital hematoma or due to a direct injury. This is a serious complication often resulting in permanent visual loss.